About Me
Physician · Biomedical Engineer · Implementation-Minded Strategist
I'm Tahir Hafeez Malik, MD, a pulmonary, critical care, and sleep medicine physician at Mount Sinai with a background in biomedical engineering, global health, outcomes research, and health system implementation. My work has consistently focused on one question:
How do we take promising healthcare ideas and determine whether they are clinically meaningful, operationally feasible, and ready for real-world implementation?
That question is the foundation of SunriseMD.
My path into medicine started through engineering. At Rice University, I studied bioengineering with a focus in global health technologies. At Baylor College of Medicine, I continued that work through health policy, global health, quality improvement, and clinical research. I later trained in internal medicine at NYU and am now completing fellowship in pulmonary, critical care, and sleep medicine at Mount Sinai, where I also serve as Chief Fellow.
Across those experiences, I have built a practical framework for evaluating healthcare innovation: understand the clinical problem, assess the evidence, pressure-test feasibility, and design for implementation.
Biomedical Engineering & Device Design
Building Around Clinical Need, Cost, and Durability
Before becoming a physician, I trained as a biomedical engineer. That background taught me to approach healthcare problems by first understanding the user, the environment, the constraints, and the failure points.
At Rice, I helped develop PneumaShoe, a low-cost, durable intermittent pneumatic compression device designed to prevent venous thromboembolism in low-resource settings. The project required more than technical design — it required understanding clinical workflows, cost constraints, durability requirements, and the realities of deployment in settings where conventional medical devices may be too expensive or difficult to maintain.
The project received multiple recognitions, including:
- Rice Department of Bioengineering Outstanding Senior Design Project Award
- 2017 Willy Revolution Award for Engineering Innovation
- Selection for the Design of Medical Devices Conference Student Design Showcase
- Selection for the Rice 360° Global Health Design Competition
- 3rd place at the National Biomedical Engineering Society Undergraduate Design Competition


That experience shaped how I think about innovation: a device, tool, or intervention is only as valuable as its ability to solve a real problem in the environment where it will actually be used.
Global Health & Implementation Science
Designing Interventions Around Real-World Constraints
My global health work has focused on a central implementation question: how do we design healthcare interventions that are not only evidence-based, but feasible in the environments where they need to work?
Malawi & The Gambia — Field Work in Low-Resource Settings
Earlier in my training, I worked on global health projects in Malawi and The Gambia that taught me how to approach clinical problems through the lens of local context. In Malawi, I investigated failure modes in oxygen concentrators and helped design durable, locally sourced engineering solutions for low-resource settings. In The Gambia, I helped develop needs assessments and surveys to evaluate maternal and newborn safety workflows across rural and urban clinical sites.
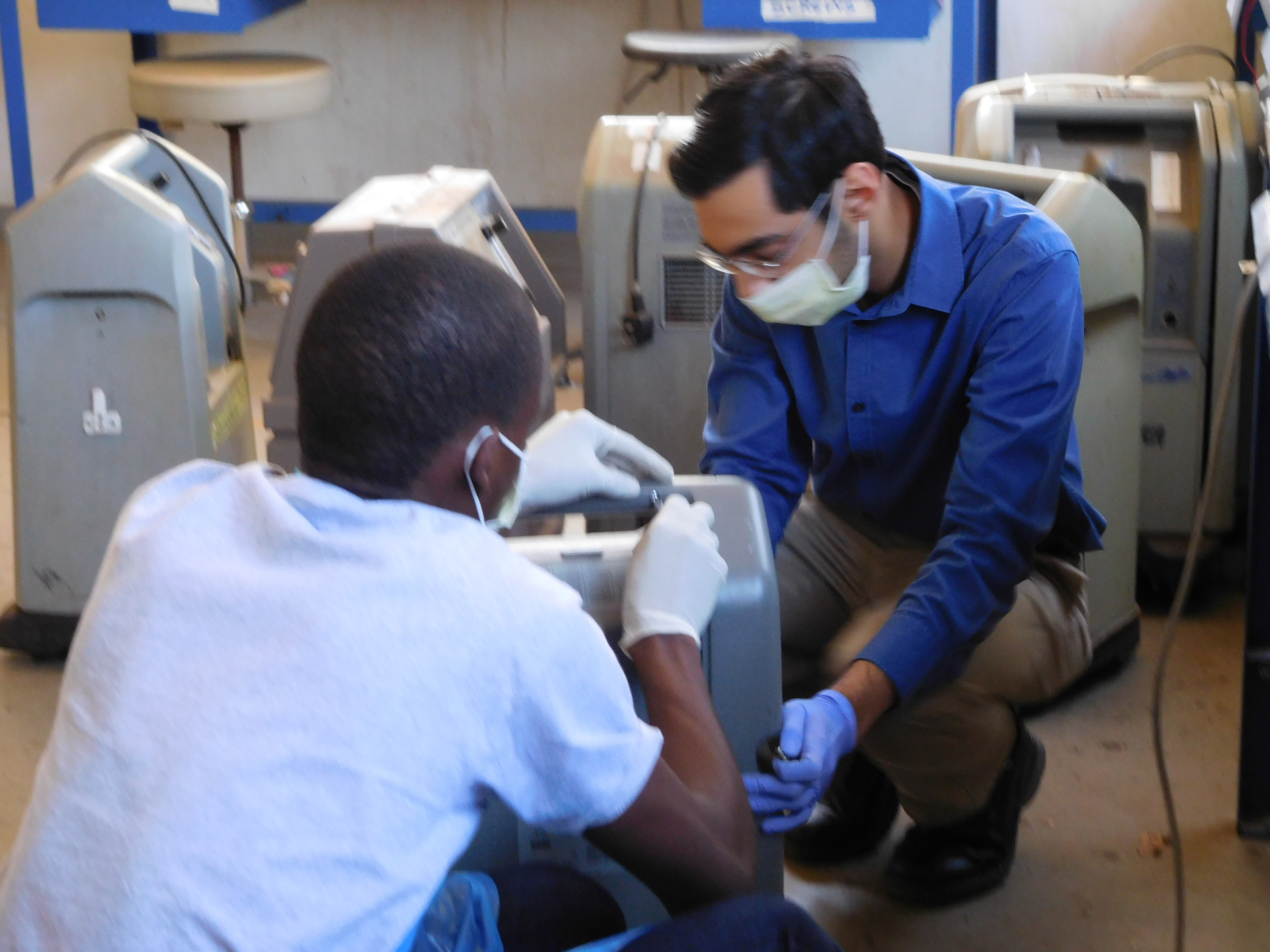
NYU — Implementation Research in India
During residency at NYU, I worked with Dr. Rajesh Vedanthan's global health lab studying whether air purifiers could affect the progression of heart failure in India. As part of the Exposures Committee, I helped design study protocols with long-term human-resource and financial constraints in mind. Through the Capacity Building Committee, I contributed to coursework and SMART goals intended to strengthen local research infrastructure in India.



Together, these experiences shaped how I evaluate healthcare innovation today. A promising idea is only meaningful if it can survive contact with real-world constraints: staffing, cost, culture, infrastructure, incentives, and the daily workflow of the people expected to use it.
Outcomes Research & Clinical Due Diligence
Evaluating High-Stakes Decisions with Evidence
My research has also focused on high-stakes clinical decisions where data, uncertainty, and resource constraints intersect.
In transplantation, I helped develop organ discard risk indices designed to better understand why donor organs are accepted or discarded. This work included research on pediatric liver allograft discard, heart transplantation discard risk, and machine-learning approaches to donor lung discard.

This research strengthened the way I approach due diligence in healthcare. When evaluating a clinical product, intervention, or system-level strategy, the key questions are rarely just, "Does this work?" The better questions are:
For whom does it work? Under what conditions? Compared to what? At what cost? And what would it take to implement it safely and sustainably?
Those are the questions that connect outcomes research to real-world decision-making.
Management & Cross-Functional Leadership
Turning Ideas into Coordinated Action
Healthcare implementation depends on more than evidence. It requires coordination across people, institutions, incentives, and timelines.
Throughout my training, I have worked across multidisciplinary teams that required both operational planning and stakeholder management. During the COVID-19 pandemic, I founded and coordinated city-wide blood drives in Houston, facilitating collaboration between trauma surgery leadership, the Gulf Coast Regional Blood Center, Rice EMS, and medical student volunteers. The effort collected more than 300 bags of blood across five drives during a period of national shortage.
I have also led student, research, and clinical teams, including serving as Chief Fellow at Mount Sinai. These experiences have helped me understand that implementation is not simply about having the right idea — it is about building the structure, relationships, and execution plan needed to make that idea work.
Why SunriseMD
SunriseMD is built around the perspective I have developed across engineering, medicine, global health, implementation science, and outcomes research.
I believe healthcare innovation needs disciplined evaluation. New technologies, clinical programs, and AI-enabled tools should not be judged by novelty alone. They should be evaluated by whether they address a meaningful clinical problem, whether the evidence is strong, whether the implementation pathway is realistic, and whether they can improve care without adding unnecessary complexity.
My goal with SunriseMD is to help bridge that gap: translating evidence into strategy, strategy into implementation, and implementation into measurable clinical value.